Removing barriers. Finding resources.
Vivor empowers health care providers to connect patients with the financial resources they deserve.
Removing barriers. Finding resources.
Vivor empowers healthcare providers to connect patients
with the financial resources they deserve.
Vivor aims to improve your treatment experience. Learn how you can work with your provider to reduce your out-of-pocket costs.
Our platform directly addresses
financial toxicity. Find out how your organization can improve patient experience and reduce bad debt.
Vivor bridges the gap between
patients and financial assistance. Discover how our platform supports initiation and adherence.
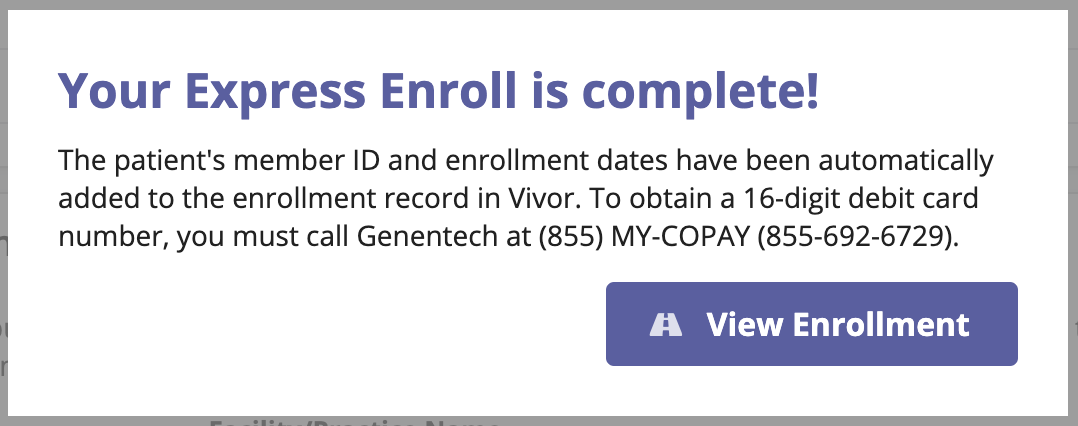
Featuring Express Enroll
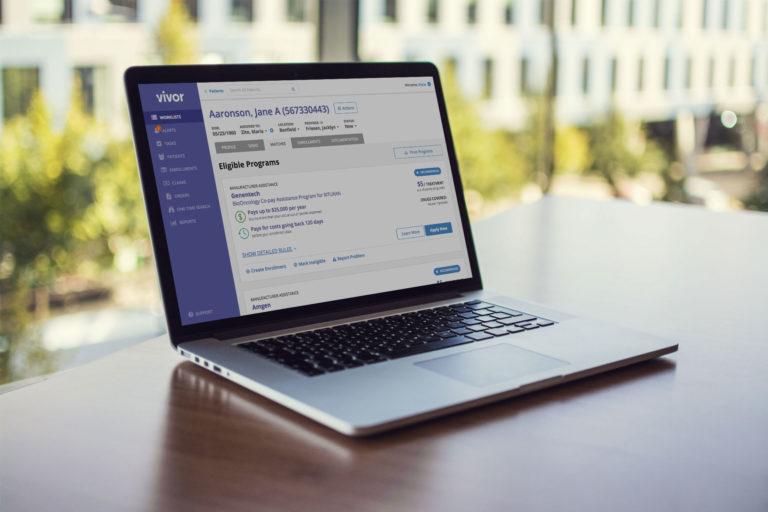
Vivor’s newest feature enables you to secure financial assistance faster than ever, by completing a real-time and fully electronic enrollment from directly within the Vivor platform. No duplicate data entry. No extra usernames and passwords to remember. And most importantly, fewer barriers to care for your patients.
Now available for co-pay assistance and free/replacement programs supporting over 30 of the most commonly used products in oncology—with many more coming soon. Schedule a demo today to learn more about this exciting new capability.
Vivor’s cloud-based platform connects patients to the financial assistance they need by helping providers to find and manage resources.
Explore how your organization can join the growing number of Vivor customers.
LATEST News
PRNewswire
July, 2021
Vivor.com
April, 2021
Vivor.com
August, 2020
